|
|
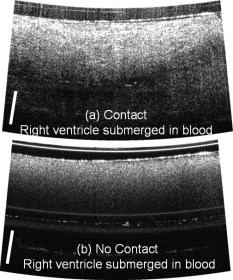
1.IntroductionCardiac arrhythmias are a major source of morbidity and mortality in the United States.1 Radio-frequency ablation (rfa) directed at interrupting critical components of arrhythmia circuits is the standard of care for the treatment of tachyarrhythmias. Current techniques for anatomical guidance of ablation therapy utilize low-resolution 2-D fluoroscopic images or static images from computed tomography merged onto fluoroscopy. Monitoring of rfa is by indirect means, such as assessment of tissue temperature, power delivery, and impedance at the tip of the ablation catheter. This indirect method of monitoring can often result in delivering more rfa lesions than necessary to achieve a therapeutic effect, prolonging procedure times and thereby increasing the risk of these procedures. Intracardiac echocardiography monitors rfa therapy in real time to assess catheter-tissue contact and contact angle,2 visualize stenosis of pulmonary vessels2 and embolic events. However, intracardiac echocardiography does not have sufficient contrast to visualize the formation of rfa lesions. Additional technology for directly monitoring ablation lesion formation during procedures in real time can further decrease procedural time and improve patient and operator safety. Optical coherence tomography (OCT) is an emerging modality that provides high-resolution, depth-resolved imaging of tissue microstructures.3 OCT has demonstrated the ability to distinguish ablated from untreated tissue,4 and image the atrioventricular node,5 and abnormal fiber organization5, 6 within ex vivo cardiac animal models. To translate OCT technology, optical catheters have been developed for imaging internal structures, and have been used for gastrointestinal endoscopy7 and intravascular imaging.8 A variety of designs have been employed including forward-imaging9, 10, 11 and side-viewing catheter.12 Designing a forward-imaging catheter that is both small in diameter and flexible presents many challenges. Others have designed probes with distal actuation to provide a wide range of scanning patterns.9, 13, 14 However, these catheters are not easily miniaturized, as the scanning mechanism limits the outer diameter of the catheter tip. Proximal actuation has been shown,10 but the probe was rigid. In this work, we present real-time imaging of rfa lesion formation and imaging in the presence of blood with a flexible, forward-imaging OCT catheter. 2.Methods and ResultsCardiac rfa lesions are formed most effectively if the ablation catheter is perpendicular and has adequate contact with the tissue. Therefore, a flexible forward-scanning OCT catheter was designed and prototyped that allows for in-contact, circular-scan imaging (Fig. 1 ). Light is delivered via a SMF28e optical fiber, the beam is focused by a GRIN lens, deflected off-axis by a Risley prism, and a fused-silica optical window isolates the probe interior from the tissue environment [Fig. 1]. The mechanical support was designed from glass, ceramic, and polymer materials (no metal) to avoid thermal effects and interference in close proximity to the rfa catheter [Fig. 1]. Rotary motion imparted by torque applied to the fiber proximally, at the fiber rotary joint, allowed for circular scanning. The rigid portion of the catheter was in length and the outer diameter was . Polytetrafluorethylene moisture seal heat shrink tubing was placed on the probe end cap, increasing the outer diameter at the probe tip to . The spot diameter of the design is full-width at half-maximum (FWHM), with minimal aberrations over of axial scan range from the optical glass [Fig. 1]. Spot profiles measured using a beam analyzer [Fig. 1] were circular, clean, and under . Fig. 1OCT forward-imaging probe. (a) Schematic of probe for circular scanning, GRIN lens used for focusing, Risley prism to deflect beam off axis, optical glass to isolate probe from environment. Rotation of assembly produces circular scanning. (b) Close-up of proximal end of probe. (c) Spot profile from ASAP simulation and (d) measured from prototype catheter showing a FWHM spot size. (e) In vivo human skin image at . scale bar. 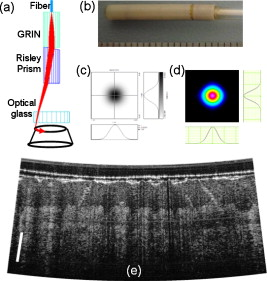 The forward-imaging catheter was integrated into a Fourier domain OCT system.15 A superluminescent diode centered at with a (FWHM) bandwidth was used for the light source (Inphenix, Livermore, California). A linear in wave-number spectrometer15 was used to project spectral interference fringes onto a InGaAs line-scan camera (Goodrich, Princeton, New Jersey). The system had a imaging range, fall off, signal-to-noise ratio, and axial resolution (in tissue). An image of in vivo human thick skin taken at 10 frames per second (fps) with 4000 lines per frame (lpf) is shown in Fig. 1. Visualizing real-time ablative lesion formation using the forward-imaging catheter was demonstrated using ventricular wedges from a freshly excised swine heart. Following the onset of general anesthesia, a lateral thoracotomy was performed, and the heart was rapidly excised and placed in ice-cold phosphate buffered saline (PBS). Individual sections of left ventricular muscle were placed in a custom chamber with PBS maintained at . The OCT forward-imaging probe was bound side by side to the rfa catheter [Fig. 2 ] and imaging was conducted at with 2000 lpf. Imaging was conducted for , prior to the start of rf energy delivery, during energy delivery, and after the conclusion of energy delivery [Fig. 2]. RFA lesions were created with a temperature-controlled protocol with a maximum delivered power of using the Maestro 3000 generator and 8-Fr, tip catheter Blazer II (Boston Scientific, Natick, Massachusetts). Staining with 1.0% triphenyltetrazolium chloride in PBS for at was used to validate lesion formation [Fig. 2]. Baseline images show a birefringence-dependent dark band characteristic of healthy, untreated myocardium [Fig. 2]. With the application of rf energy, the band broadens and appears deeper in the tissue [Figs. 2, 2, 2]. It is important to note that the rf energy, and the temperature rise during energy delivery, did not affect the image quality nor the mechanical stability of the catheter. Fig. 2Visualization of dynamics due to rf energy delivery. (a) Samples placed in custom chamber with superperfusion flow of PBS. Forward-imaging catheter bound side by side to rfa catheter. (b) OCT imaging conducted over 90 sec and of rf energy delivery. (c)-(f) OCT images at 10, 20, 70, and . Baseline images characterized by birefringence artifact band (arrows). With the application of rf energy, location of birefringence artifact bands lower and then disappear. Scale bar . Region closer and further from rfa catheter labeled as C and F, respectively. (g) TTC vital staining, necrotic tissue white and viable tissue red. (Color online only.) 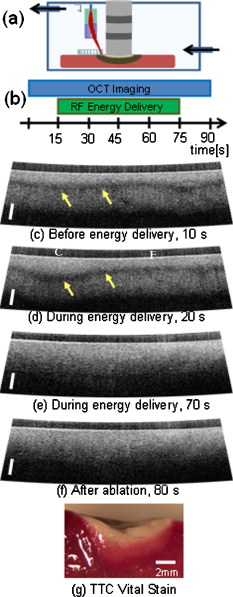 The effect of the presence of blood was evaluated by imaging the ventricular wedge submerged in heparinized swine blood. An image of the myocardium was obtained when the catheter was in direct contact with the tissue, displacing the blood (Fig. 3 ). Blood strongly attenuates light at . When the catheter probe was not in direct contact with the tissue, the imaging depth was significantly reduced [Fig. 3]. An important factors that affect lesion size is the maintenance of tissue-rfa electrode contact. This visual feedback could allow assessment of contact. 3.Discussion and ConclusionWe demonstrate a flexible forward-imaging OCT catheter made without metal that provides circular scanning by proximal actuation of the fiber. Using a forward-imaging catheter, we show that OCT can provide real-time direct visualization of rfa therapy, assessing tissue-electrode contact visualizing lesion formation, and can image in the presence of blood. The current design is optimized for the case when the rf catheter has adequate near-perpendicular contact with the tissue surface. For nonoptimal cases, contact angle can potentially be determined by detecting the surface position as a function of rotation angle. This probe design can be miniaturized and integrated into a rfa catheter for future in vivo use, and adapted to other applications where a miniature, flexible forward-imaging OCT probe is needed. A direct image by OCT also has the potential to guide the precise application of rf energy, and to identify normal cardiac structures where ablation could be harmful. Importantly, this advance in catheter technology can decrease the procedural time and radiation exposure to the patient and physician. Video 1Real-time visualization of dynamics due to rf energy delivery. Baseline imaging of before the start of of RF energy delivery on the Endocardium of the left ventricle (QuickTime ). .  AcknowledgmentsThe authors thank Steve Schomish for his technical assistance and Avo Photonics for prototyping the catheter. The project was supported by the Wallace H. Coulter Foundation and by the NIH (F31HL085939, R01HL083048, and RR1246). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Heart Lung and Blood Institute or the NIH. ReferencesW. Rosamond, K. Flegal, K. Furie, A. Go, K. Greenlund, N. Haase, S. M. Hailpern, M. Ho, V. Howard, B. Kissela, S. Kittner, D. Lloyd-Jones, M. McDermott, J. Meigs, C. Moy, G. Nicho, C. O’Donnell, V. Roger, P. Sorlie, J. Steinberger, T. Thom, M. Wilson, and Y. Hong,
“Heart disease and stroke statistics 2008 update: a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee,”
Circulation, 117 e25
–e146
(2008). https://doi.org/10.1161/CIRCULATIONAHA.107.187998 0009-7322 Google Scholar
J. F. Ren and F. E. Marchinski,
“Utility of intracardiac echocardiography in left heart ablation for tachyarrhythmias,”
Echocardiogr., 24 533
–540
(2007). https://doi.org/10.1111/j.1540-8175.2007.00426.x 0742-2822 Google Scholar
D. Huang, E. A. Swanson, C. P. Lin, J. S. Schuman, W. G. Stinson, W. Chang, M. R. Hee, T. Flotte, K. Gregor, C. A. Puliafito, and J. G. Fujimoto,
“Optical coherence tomography,”
Science, 254 1178
–1181
(1991). https://doi.org/10.1126/science.1957169 0036-8075 Google Scholar
C. P. Fleming, K. J. Quan, H. Wang, G. Amit, and A. M. Rollins,
“In vitro characterization of cardiac radiofrequency ablation lesions using optical coherence tomography,”
Opt. Express, 18 3079
–3092
(2010). https://doi.org/10.1364/OE.18.003079 1094-4087 Google Scholar
W. Hucker, C. Ripplinger, C. P. Fleming, V. Fedorov, A. M. Rollins, and I. R. Efimov,
“Bimodal biophotonic imaging of the structure-function relationship in cardiac tissue,”
J. Biomed. Opt., 13 054012
(2008). https://doi.org/10.1117/1.2975826 1083-3668 Google Scholar
C. P. Fleming, C. Ripplinger, B. Webb, I. R. Efimov, and A. M. Rollins,
“Quantification of cardiac fiber orientation using optical coherence tomography,”
J. Biomed. Opt., 13 030505
(2008). https://doi.org/10.1117/1.2937470 1083-3668 Google Scholar
D. C. Adler, C. Zhou, T. H. Tsai, J. Schmitt, Q. Huang, H. Mashimo, and J. G. Fujimoto,
“Three-dimensional endomicroscopy of the human colon using optical coherence tomography,”
Opt. Express, 17 784
(2009). https://doi.org/10.1364/OE.17.000784 1094-4087 Google Scholar
G. J. Tearney, S. Waxman, M. Shishkov, B. J. Vakoc, M. J. Suter, M. I. Freilich, A. E. Desjardins, W. Y. Oh, L. A. Bartlett, M. Rosenberg, and B. E. Bouma,
“Three-dimensional coronary artery microscopy by intracoronary optical frequency domain imaging,”
JACC: Cardiovasc. Imag., 1 752
(2008). https://doi.org/10.1016/j.jcmg.2008.06.007 Google Scholar
N. R. Munce, A. Mariampillai, B. A. Standish, M. Pop, K. J. Anderson, G. Y. Liu, T. Luk, B. K. Courtney, G. A. Wright, I. A. Vitkin, and V. X. D. Yang,
“Electrostatic forward-viewing scanning probe for doppler optical coherence tomography using a dissipative polymer catheter,”
Opt. Lett., 33 657
–659
(2008). https://doi.org/10.1364/OL.33.000657 0146-9592 Google Scholar
J. Wu, M. Conry, C. Gu, F. Wang, Z. Yaqoob, and C. Yang,
“Paired-angle-rotation scanning optical coherence tomography forward-imaging probe,”
Opt. Lett., 31 1265
–1267
(2006). https://doi.org/10.1364/OL.31.001265 0146-9592 Google Scholar
X. Liu, M. J. Cobb, and Y. Chen,
“Rapid-scanning forward-imaging miniature endoscope for real-time optical coherence tomography,”
Opt. Lett., 29 1763
–1765
(2004). https://doi.org/10.1364/OL.29.001763 0146-9592 Google Scholar
J. Xi, L. Huo, Y. Wu, M. J. Cobb, J. H. Hwang, and X. Li,
“High-resolution OCT balloon imaging catheter with astigmatism correction,”
Opt. Lett., 34 1943
(2009). https://doi.org/10.1364/OL.34.001943 0146-9592 Google Scholar
P. R. Herz, Y. Chen, A. D. Aguirre, K. Schneider, P. Hsiung, and J. G. Fujimoto,
“Micromotor endoscope catheter for in vivo, ultrahigh resolution optical coherence tomography,”
Opt. Lett., 29 2261
–2263
(2004). https://doi.org/10.1364/OL.29.002261 0146-9592 Google Scholar
K. H. Kim, B. H. Park, G. N. Maguluri, T. W. Lee, F. J. Rogomentich, M. G. Bancu, B. E. Bouma, J. F. de Boer, and J. J. Bernstein,
“Two-axis magnetically-driven MEMS scanning catheter for endoscopic high-speed optical coherence tomography,”
Opt. Express, 15 18130
–18140
(2007). https://doi.org/10.1364/OE.15.018130 1094-4087 Google Scholar
Z. Hu and A. Rollins,
“Fourier domain optical coherence tomography with a linear-in-wavenumber spectrometer,”
Opt. Lett., 32 3524
–3527
(2007). 0146-9592 Google Scholar
|